Data Visualization, JavaScript, Three.js, HTML, CSS, Arduino, Speculative Design
This is Vanessa and she is 24 years old.
A couple of years ago, Vanessa noticed a bump on her breast. She went to the doctor, and described her symptoms and concerns. She was told to put a hot towel over it over certain intervals for a period of time.
She noticed that the bump became worse while doing this. When she went back to the doctor, time had passed, and unfortunately, she was diagnosed with breast cancer.
When Vanessa was voicing her concerns during her initial doctor’s visit, the doctor brushed her concerns off thinking she was overreacting, and said that she was too young to have breast cancer. If she had been properly examined and not ignored despite her young age, she may have been able to avoid the struggle that was to come - to fight cancer.
Unfortunately, this experience is not unique to Vanessa.

The nationwide misdiagnosis rate is estimated at around 5-6%, which is around 12 million US patients per year, or 1 in 20 adults.
THE PROBLEM
The chances of a patient of color being misdiagnosed are greater than those of a white patient. Unequal medical care and quality of diagnosis received isn’t due to just location, education or income; it’s also at times due to the cognitive biases of healthcare professionals, and decades of clinical studies that examined only white, male bodies. This leads to unequal medical care for women, people of color, and minorities / immigrants.

Images of conditions on dark skin are underrepresented in educational materials. This means that med school students, and future doctors, are trained to be biased towards white skin, and aren’t able to identify conditions on varying skin tones as easily.
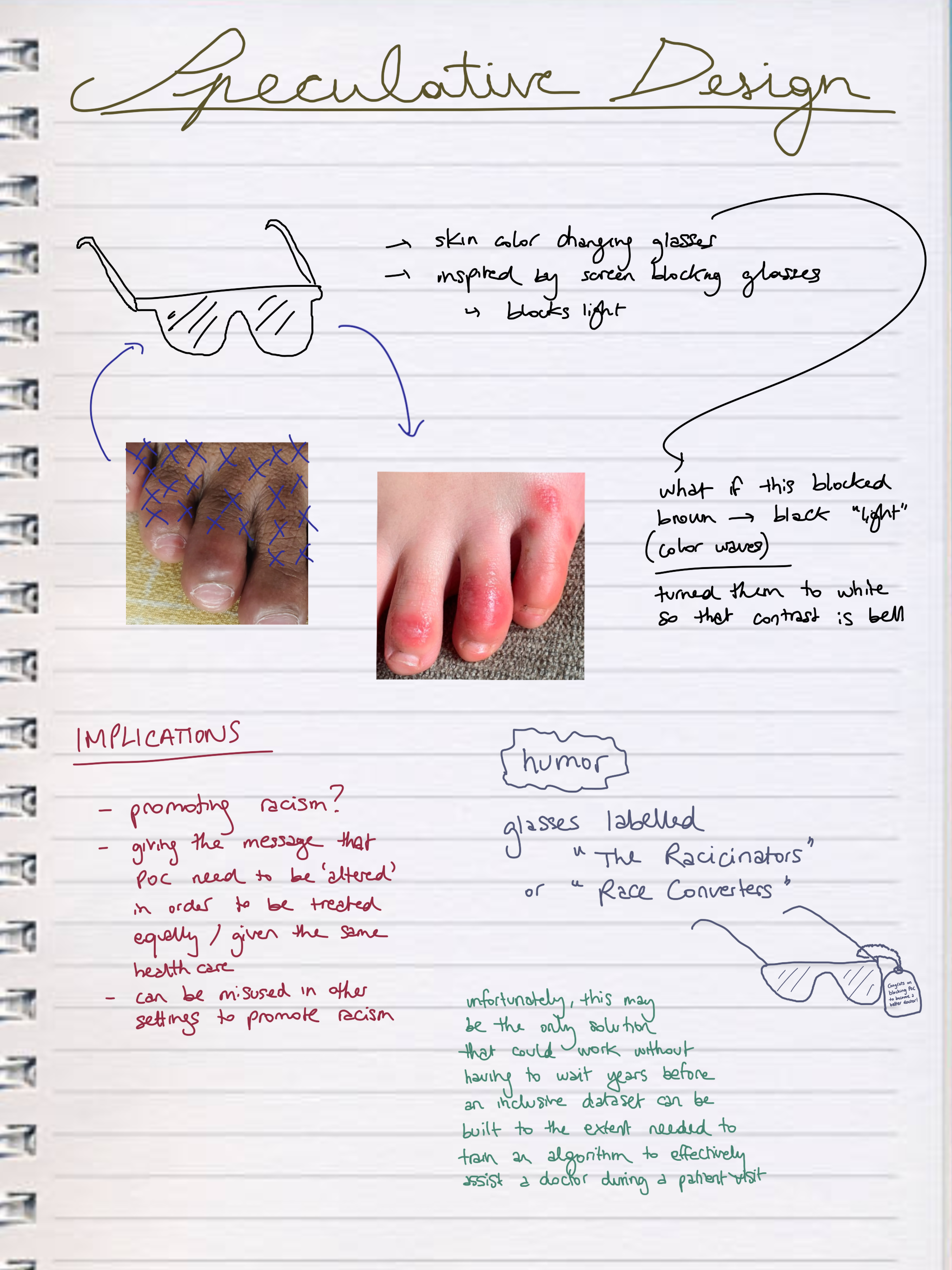
As you can see above, it’s really important to be able to train on inclusive case studies because conditions / symptoms can look very different on different skin tones.
For example, during a medical school student’s clinical rotations, a Black patient came to a clinic with a mysterious rash that had a purplish hue. No one knew what it was. A biopsy revealed it was psoriasis, a common skin condition that doctors usually diagnose on sight. Yet it often goes unidentified and untreated in people of color. Studies have shown that black patients are less likely to get certain treatments than white people with the same conditions.

If doctors aren’t able to diagnose and treat them effectively, this means that minorities are more prone to developing these conditions to more fatal stages, and are receiving a lower quality of care.
MY THESIS
My thesis is an exploration of the skin biases in healthcare, aimed to understand and uncover the various layers of the problem. Below is my journey, with an approach to the problem from 3 different subsets: (1) awareness, (2) practitioners and the healthcare system, and (3) the education system.
SYSTEMS MAPPING
I mapped out the systems and processes of this space as a first step of understanding the forces at play.
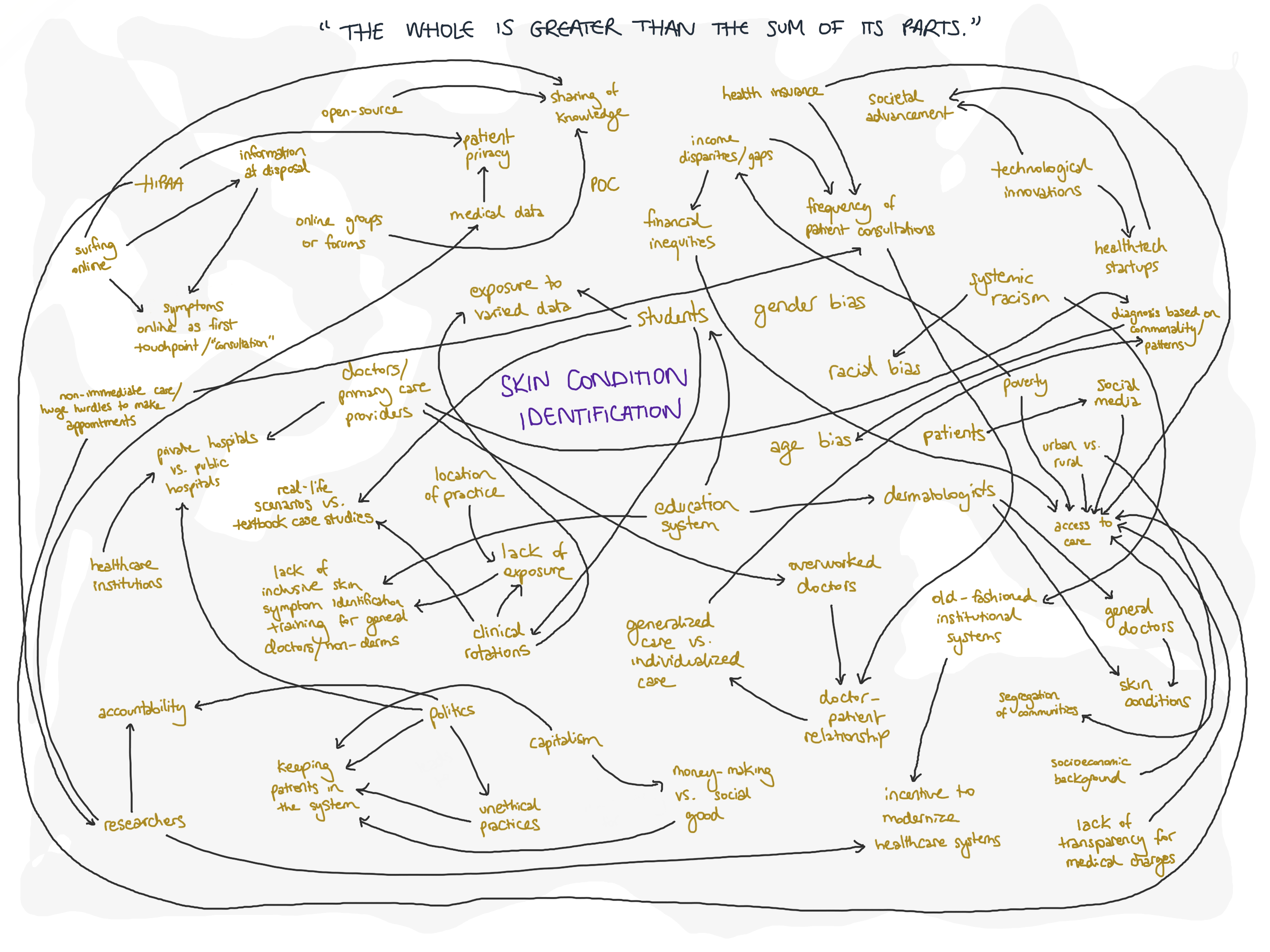
SUBSET 1: AWARENESS
As seen from the systems map, this is a big problem with a lot of layers, factors and effects. So what is the main problem I am addressing?
People that have experienced misdiagnoses, having their symptoms ignored by their healthcare providers or that have been wronged by the system don’t have a place to voice their experiences. They go through their experiences knowing it could’ve been avoided, but don’t have a voice or way to change the system on their own.
Sure, communities do exist and stories have been told.
News outlets mainly cover stories of people who have been misdiagnosed for 15+ years or critical misdiagnoses - the big stories. But the pain and injustice is real, regardless of how long your misdiagnosis lasted.
There are reddit and Facebook communities where people share these stories, but sometimes it is only part of the goal of the community, not the entire aim, or it’s not one big collective.
These problems are unknown to many- there is a lack of awareness. And awareness is the first step to effectuate change.
As a way of validating the existence of these experiences, and in turn, of the problems in the healthcare and education systems, I am creating a data visualization web experience, with two different modes, that shines a light on people’s misdiagnosis stories, as a way of forming a collective community.
EXP-MODE
The experience mode presents an island of body parts among nature. This experience aims to ignite the audience’s feelings and empathy through the audio element. It aims to form a connection between the viewer and those telling their stories.
The body parts scattered around the island each represent a misdiagnosis story submitted to the database. The user can move around and discover a body part. The wilderness around symbolizes that these stories are hidden and unknown - wild and uncultivated. The body parts are in the wild as if they were discarded, to show how unempathetic the healthcare system has been, and that it needs to change. The contrast between human and nature here shows how unnatural this bias and healthcare training processes are. This is the path to expose healthcare biases.

DATA-MODE
The data mode is a more traditional form of a data visualization, where you can learn about hover over body parts to hear individual misdiagnosis stories, and contextual information regarding the breakdown of demographics is paired with it at the top right.

The data is organized into loose clusters that mirror the chosen tab (so if you choose the gender tab, the data will rearrange itself into clusters that match the breakdown).
This experience aims to draw connections between the stories and the people behind them, and show the realities of bias in healthcare.
CONTRIBUTIONS
I’ve been collecting data by sending out a Google form to different communities of people, such as cancer groups and other diagnosis groups on Facebook.
Link to Google Form ︎︎︎

ITERATIONS
SPECULATIVE DESIGN EXERCISE
What are the current affects of the healthcare space? What can a more desirable alternative reality look like, and what are its alternative affects?

This exercise aims to conceptually develop the overall look and feel of the database. It encourages connection and harmony between current and alternative systems, as a form of imagining utopian futures.
THE LAYERS METAPHOR
Coming soon.
SUBSET 2: PRACTITIONERS & HEALTHCARE SYSTEM
SUBSET 3: EDUCATION SYSTEM
Coming soon.
ARCHIVE
